
Rewarding Careers for Nurses
On a Saturday morning, glazed with golden light canting through picture windows, DeDe Boone makes her rounds to one of five residents of a Southern Oregon group residence where the hallways are lined with family photographs and signs that announce in bold Avallon font emphatically what this place is: “Home.”
“Is Mr. Wesley up yet?” Boone says, her voice entering a space before she does as she steps straight, efficient lines into a living room where a long-time resident lays in bed, his head raised to a 30-degree angle, and pillows stuffed at his side. “Hi Mr. Wesley! How are you this morning? How did you sleep last night? Should we check your tube?”
Boone snaps on a fresh pair of Latex gloves and checks and adjusts Wesley’s breathing tube. His eyes pinball across the room as he tries to follow Boone’s voice before he swivels his neck and arches his eyebrows, trying to track her.
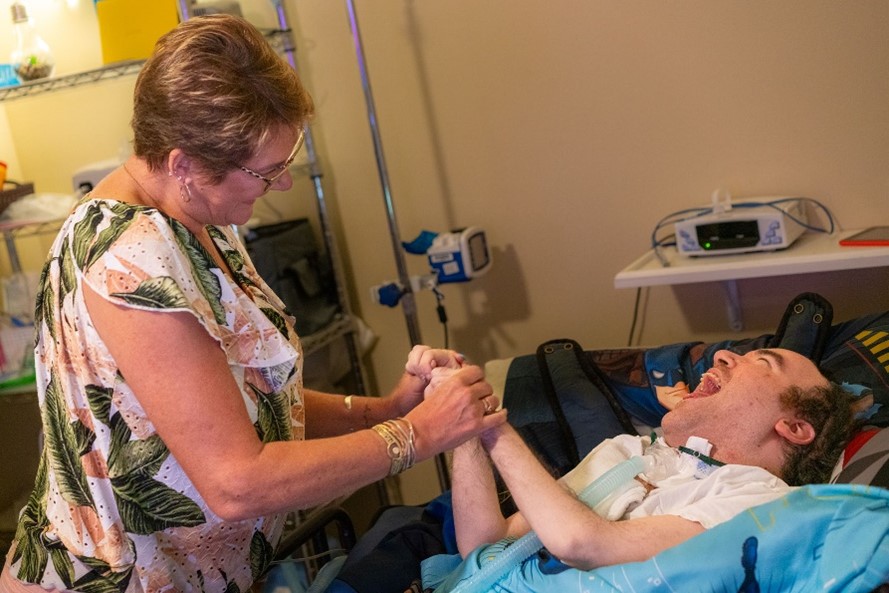
Boone clears his tracheotomy tube and lays it back in place before snapping off the plastic gloves and tossing them into the trash. Then, she does something simple but meaningful for her patient; she dispenses morning medicine along with love and affection. Boone leans against Wesley’s bed railing, takes his hand and caresses it, then brushes back his bangs and tickles his sides—all of it in the seamless arc of a single movement. Suddenly, Wesley’s face bursts open into an 800-lumen light smile and the room comes alive with color.

“There it is, there’s your smile!” Boone says, as the pair hold a gaze for a few short beats, communicating without words. There is another language at play here—one built on instinct, nonverbal cues and a basic human desire to connect.
“Getting an individual to smile, that’s my paycheck.”
Nurses like Boone are a cornerstone to providing critical care to individuals with disabilities, and in the case of Boone’s patients, individuals also deemed medically fragile.
A severe nursing shortage across the healthcare industry, compounded with pandemic-triggered burnout among many in the health-care industry, has left an abundance of job opportunities within the I/DD field.
While being a nurse in the I/DD field comes with unique challenges, it also comes with just as many unique and compelling rewards—a message nurses who already work in this field hope to amplify for nurses in other fields, such as hospital nurses, who may be seeking a career shift, as well as for future nursing recruits in school who may be considering nursing careers. They cite flexible hours, the opportunity to build relationships and the altruistic aspect of having a positive impact on another person’s life as special benefits to working in the I/DD field.
And, they say, if you can find the right position where your experiences and your personality line up with the job, you could have one of the most meaningful and enriching careers of your life.
"The absolute best part is after all their problems are solved, at least for a short time, you get to see people at their best."
“You get to know the individuals. You’re not just meeting them for one or two shifts and discharging them,” said Brian Wenger, a nurse who recently left a hospital job to work at the state’s Stabilization and Crisis Unit, where he provides care to youth in group home settings. SACU nurses work across multiple counties from Gresham to Eugene to care for individuals who have both an intellectual and/or developmental disability and mental health issues. “The absolute best part is after all their problems are solved, at least for a short time, you get to see people at their best. You get to see their potential and see them grow and change. You can attend their birthday parties or movie nights and cooking classes. You don’t get those moments every day but they happen often enough where this is a pretty unique job and we’re lucky we get to do it. I tell people I have one of those unicorn types of jobs.”

A significant variety of distinct career tracks and positions currently available within the I/DD field makes finding the right position easier. Nursing opportunities can be found in both in-home support services that allow individuals to live in their own home as well as 24-hour residential support services in a group setting. Specialized career paths in I/DD include:
The Children’s Intensive In-home Services (CIIS) Program, which provides family-sensitive and culturally sensitive case management services to support families as they care for their children with significant disabilities in their own homes, including a medically fragile program for children who rely on specialized medical technology for their health and are cared for by private duty nurses, who are nurses or skilled caregivers overseen by RNs;
The Long-term Care Community Nursing (LTCCN) Program in which RNs provide in-home care such as teaching the individual or family member how to perform nursing tasks, health education for the individual, family members, caregivers or foster home providers and a nursing assessment with medication review and service plan for each individual
Direct Nursing Services (DNS) which provide shift nursing to adults age 21 and older with complex health management support needs that require ongoing assessment and reassessment, supervision, nursing treatments, therapies and interventions either in their own home or a foster home.
24-hour residential group home nursing where RN’s and LPN’s assist adults with medical support needs who are living in licensed group homes. Certified and endorsed agencies who operate the homes hire nurses directly. Nurses like Boone are working hard to ensure the needs of individuals are being met. However, like many nursing fields, the I/DD field faces the reality of a nursing shortage that could potentially cause some group homes to close.
If the nursing shortage continues, individuals with I/DD would face challenging scenarios in accessing support and services that help them thrive. Individuals may be admitted to nursing homes that lack specialized care, hospital emergency rooms that are likely to be already severely understaffed, or worse, unhoused on the streets.
“When we don’t have nurses in the field to take care of these individuals, the only other resource are the hospitals, so these individuals are filling up hospital beds meant for those that are critically ill,” said Lizz Pierce-Green, a SACU nurse. “Now we see hospitals with units closed because there are not enough nurses to staff those units. And that just causes a backup and then a flood and then what happens is we’ve got people on the streets. It becomes a vicious cycle.”
The challenge to finding adequate nursing care is not specific to the I/DD professional sector, but nurses who work with individuals with disabilities say the shortage is especially acute in I/DD due to lack of education and awareness about individuals with I/DD.
It’s a sentiment echoed by national-level leaders working to advance the care and rights of individuals with I/DD.
“Everyone is really stressed and strained,” said Dr. Hoangmai Pham, director of the Institute for Exceptional Care, which advocates for improved and equitable healthcare for I/DD individuals.
Pham says an added complexity to establishing adequate nursing levels for the I/DD population is “the nature of the work and how demanding and draining it can be.”
Nurses need support, reasonable working hours and time to rejuvenate, “Especially when you’re talking about I/DD, that’s giving them aides and giving them the right equipment to get through the day,” Pham said.

Reasons for Entering the I/DD Workforce
The path for nurses to get one of these rewarding jobs is as varied as the personal backgrounds of the nurses themselves. Some describe the career as a calling, coming from families with generational legacies of healthcare work, while others arrived into the I/DD field after getting burnt out in hospitals. Other nurses were compelled by personal motivation, with a loved one who has disabilities.
It’s a field where the greatest payoff comes from the people, nurses say.

“There is nothing more rewarding than walking into somebody’s home and being a part of their daily life and being the consistent person to promote overall wellness,” Pierce-Green said.
For nurses like Boone, there is both a personal imperative along with a professional calling to do more than manage the well-being of her patients; she works to see them thrive. Boone is lead nurse for a collection of 13 state-funded residential care homes in Roseburg, Ore., where individuals with intellectual and developmental disabilities receive care from a team of specialized nurses and caretakers. One among those homes is dedicated specifically for medically fragile individuals who require round-the-clock care.
Boone has taken residents on trips to the Oregon Coast, Disneyland, and into the wilderness for camping. She has learned who loves Latin music videos, Oregon Ducks football, and daytime soaps. And she knows, with the kind of acuity and spidey sense that seems specific to mothers and skilled nurses, when a resident is either flailing or flourishing.
Cindy Duran, a nurse manager who supervises a team of 49 nurses, specialists, technicians and site managers at SACU, is inspired by the passion, leadership and self-direction she has observed among I/DD nurses.
“A lot of our nurses have a personal investment working with our I/DD population, and making sure they receive care like any of our Oregon citizens,” said Duran. “I don’t think people realize how important a role nurses play in the I/DD field. Nurses don’t just play a medical role. We are advocates. The glue for that entire team caring for individuals with I/DD is your RN.”
"There is nothing more rewarding than walking into somebody’s home and being a part of their daily life and being the consistent person to promote overall wellness."
Here’s a glimpse into the roles of a few of our nurses who work with individuals with disabilities:
Long-term Care Community Nursing (LTCCN) Program
Tracy Luttrell
For years, Tracy Luttrell worked from home as a graphic designer after life and love interrupted her early dreams of going to Stanford and becoming a cardiologist. She spent her early years growing up in the San Francisco Bay Area, and eventually moved to Texas when she was 17-years-old, where she got both a husband and a GED.

Tracy Luttrell recharges her batteries during lunch at a local park.
If life and love anchored her for a time in Texas, it was family that led her to Oregon and loss that launched her into a journey working with I/DD populations.
In 2011, Luttrell’s older sister became ill with an infection and ended up at Oregon Health Sciences University (OHSU), where, instead of being treated and going home, she developed toxic shock when the antibiotics used to treat her caused her liver to fail. She was 42-years-old when she died, and Luttrell was devastated. Her sister left behind four children, two of whom have developmental disabilities.
It was that loss, coupled with becoming the legal guardian of one of her nephews who has an intellectual disability, that inspired Luttrell to search for ways to honor her sister’s life and legacy.
“My sister had a master’s degree and was a teacher in special education,” Luttrell said. “I thought, ‘Let me see if I can get into that.’”
In 2014, Luttrell applied for only one nursing program and was accepted, which is how she came to enroll in the very same hospital where her sister had passed away three years prior.
Luttrell wasn’t sure what a career in caregiving for people with I/DD would look like and she all but stopped thinking about it when she graduated with her nursing degree and began working in critical care at Salem Health Hospital, where she and her family had eventually relocated after a short stint living in Southern Oregon.
“I always wanted to do ER and trauma and all that kind of stuff,” Luttrell said, which she did, along with working in the float pool where she rotated to various units of the hospital. “There was an adrenaline piece to the ER. It was exciting and the camaraderie was really good.”
But after four years in critical care at Salem Health Hospital, the hours and the pressure, and then an unexpected knee injury that hampered her mobility, took their toll.
“The stress built up,” Luttrell said. “I had a hard time sleeping, and not being able to shake off some of the things I had to deal with and decisions that had to be made and seeing people suffering and not being able to help. Some of them were suffering alone because they had no family.”
Around the time she started to feel burnt out, a colleague announced that a company that manages group homes in McMinnville needed a part-time nurse to work six hours a week. Intrigued by the job but unaware of its scope, Luttrell applied.
The agency, it turns out, operates group homes where individuals with intellectual and/or developmental disabilities live independently with a team of caregivers who help provide a safety net to support them in maintaining their health and well-being.
Luttrell currently works as a contract nurse and oversees five independent living homes and a total of 50 individuals. Her job is to support the non-licensed caregivers who help the individuals, keeping track of each individual’s medical needs via client care plans and delegating certain basic tasks that don’t require a nursing license and that caregivers are approved by the state to perform, such as giving pills to individuals or cleaning out an individual’s ears with drops.
“How I get a client is I get a referral from a case manager and I go meet with them. I look at what does their living environment have? What kind of teaching is going to be needed for the people who take care of them? Are they family members or are they non-family members who need delegation? You’re thinking about the rules and you’re thinking about what the patient is going to need,” Luttrell said.
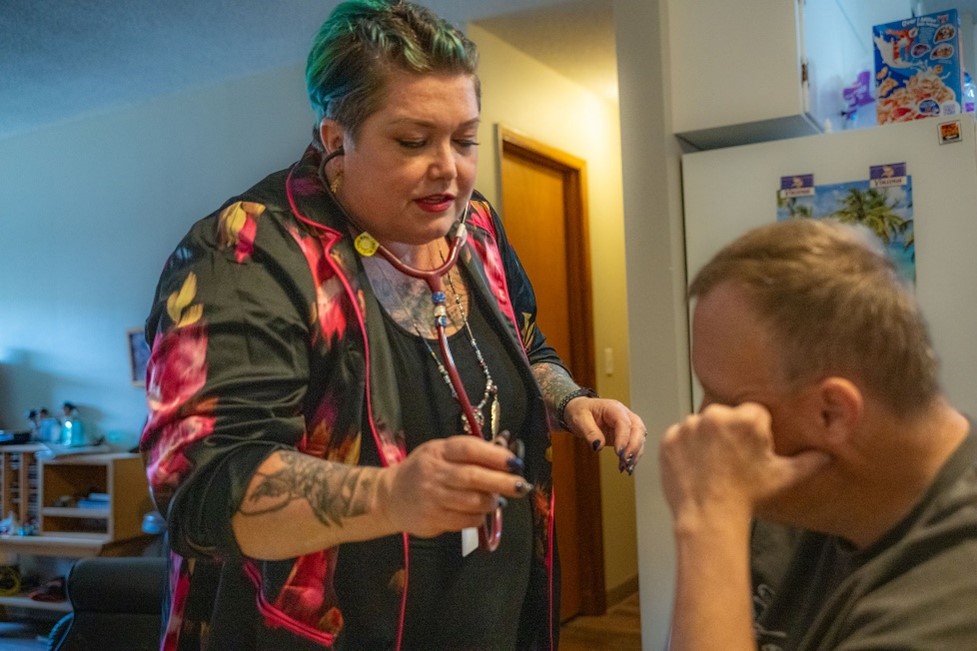
On a recent Monday afternoon, Luttrell is making the rounds to check up on a few of her clients in an independent living complex on the edge of downtown McMinnville, where a dozen apartments encircle a common courtyard and small but thriving flower gardens grow in a few of the residents’ fountain beds.
Luttrell visits Anne, who has just returned from a brisk walk in the neighborhood. Anne’s corner unit is spotless and tidy with two leather armchairs positioned in front of the TV where she and her husband watch Seahawks games. Luttrell checks her oxygen levels and her blood pressure, then presses a stethoscope to her chest to listen to her heart.
“How’s your heart Anne?” Luttrell asks, bending her body to check up on Anne as she gently rocks in her recliner.
“My heart’s great!” Anne says, beaming as she announces she’ll get to have lunch with one of her friends the next day.
When Luttrell leaves Anne’s home, she checks in with Anne’s case manager to get an update on how Anne is doing overall—information that Luttrell will later log into a system she created to track her clients’ health.
One of the greatest benefits of working in an administrative capacity in the I/DD field is the flexibility she has with her hours, Luttrell says. Once she makes her rounds, she often heads to a coffee shop or the city park, where she inputs data, reviews records and completes documentation for the day. With 50 clients on her roster, Luttrell has found ways to stay organized and still manage to conduct home visits to two or three clients per week.
But she says more nurses are needed.
“The need is so high,” Luttrell said. “I have people constantly asking me, ‘Can you take another?’ and I say, ‘No.’”
As she ducks into and out of three other homes to check up on additional clients, Luttrell takes a moment to consider her work and the consequences of not having enough nurses throughout the I/DD field to support individuals. “Helping individuals have a higher quality of life, that’s the goal. Staying home and not having to go to a facility means they live longer if we can help them manage their chronic stuff,” Luttrell said. “What kind of life would that be if you can’t get help? They would end up in a skilled nursing facility that has a long-term bed. They have care there, but it’s not your house. It’s not your garden. They deserve the same quality of life that I have. They just needed a little help getting there.”
Direct Nursing Services
DeDe Boone
DeDe Boone’s path to working as a nurse with individuals with I/DD is paved with a childhood steeped in displays of family love and affection, a penchant for numbers, and ultimately, a profound loss due to cancer.
Boone was born and raised in Roseburg, where she eventually met and married her husband, Frank. Together, the pair owned and operated a tattoo and body piercing shop while Frank built motorcycles on the side. They had a dream: they would open a motorcycle shop and Boone would be the bookkeeper.
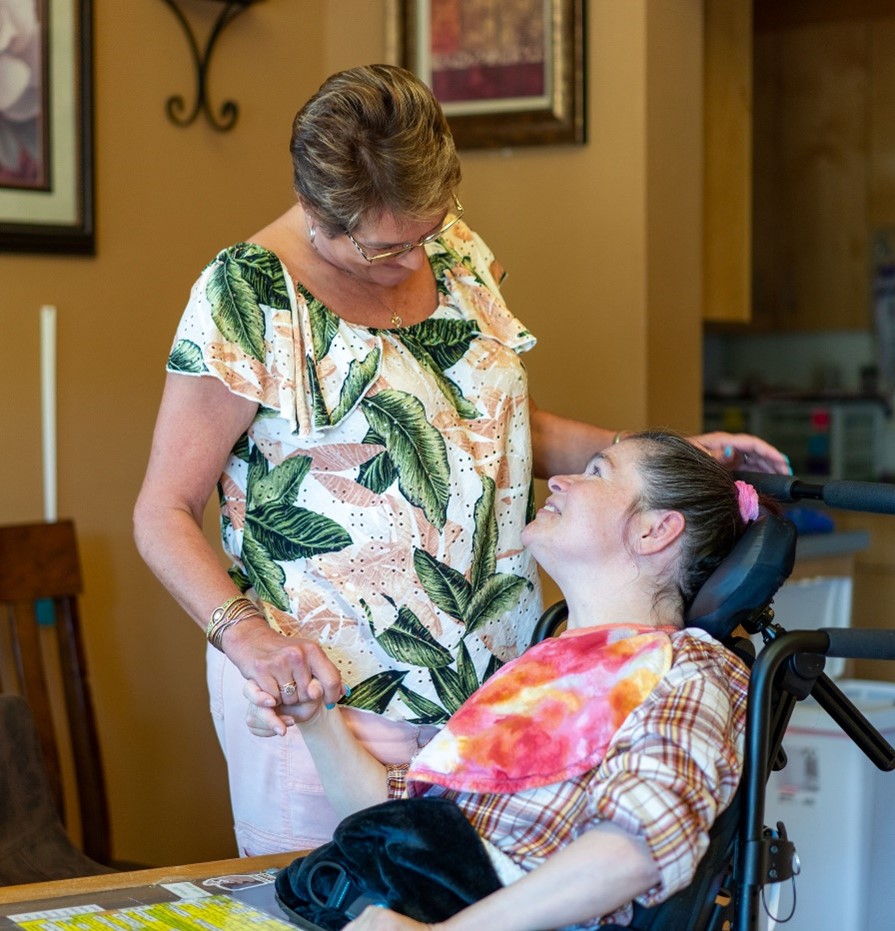
DeDe Boone and Diane connect in a number of ways.
“I love numbers,” Boone said. “We were going to make this dream happen.”
Going back to school to get a graduate degree in accounting was a logical next step and so she enrolled at Umpqua Community College. By June 2004, after reaching the end of her accounting program, she was confronted with the painful paradox of both a new beginning and the beginning of an end: she graduated with her degree, and days later, Frank was diagnosed with cancer. He passed away 17 months after she graduated.
Five years later, Boone wasn’t sure what she was going to do with the rest of her life. That’s when her mother reminded her of Boone’s very own words she had uttered while caring for Frank: that if she ever got the chance, she would become a nurse.
“I never really thought I was capable of being a nurse,” Boone said. “I knew it was a challenging career. I didn’t know I could handle the blood and the IV until my husband got sick with cancer. I started taking over his care. He was in the VA and I got a lot more experience taking care of him than I would at a normal hospital. That’s when I decided, ‘I could do this as a job.’”
She returned to Umpqua Community College, this time in the school’s nursing program, clear-eyed about her intentions and still reeling from the devastating loss she had endured: “I was going to be a hospice nurse,” Boone said.
Boone was 52 years old when she completed her nursing degree in 2012, the oldest person in her graduating class. But that fact didn’t deter her. She had a goal and plowed ahead to reach it.
Unlike many of her nursing school peers who took jobs in hospitals, Boone instead worked at the Clackamas County Jail, for a tribal clinic, and for a long-term care facility before joining Umpqua Homes in June 2018, first as a floor nurse, and eventually becoming lead nurse and overseeing 13 group homes.
In hindsight, working with individuals with intellectual and developmental disabilities may have been part of her life’s journey all along.
“I’ve always wanted to take care of people,” Boone said.
Boone said to be successful as a nurse working with individuals who have intellectual and developmental disabilities, “You have to have a heart. You have to be a giving and loving individual who is willing to give of yourself. You can’t teach someone how to care. I think you have to be born with it.”
There is a particular kind of knowing that nurses like Boone have, a keen awareness of others honed by years of experience and an innate sense of humanity. Part of this, Boone says, comes by just taking the time to get to know the individuals in your care.
“They can’t talk. They can’t tell you how they feel,” Boone said. “It’s just knowing your people and being able to talk without words and to listen without hearing.”
After spending a bit of time visiting with Wesley on her morning rounds, Boone went to a front family room with a TV mounted high in a corner. She sat in a chair next to another individual, Diane, who stays in a wheelchair during the day and communicates with a homemade sign board.
As Boone reties Diane’s pony tail, and later holds Diane’s hand, she notices Diane pointing to the word “confused” on her board.
“You’re confused why there’s a reporter and photographer here?” Boone says to Diane. “Remember we talked about this yesterday? They’re doing a story to try to get more nurses to come help us out. Isn’t that great?”

Diane’s face opens into a big smile as she shifts and bucks in her wheelchair with excitement.
Although Boone says the homes she oversees are currently fully staffed, she expects to need nurses as part of the ebb and flow of retirement and nurses going on vacations or family leave or leaving for other careers. Boone says the benefits of working in this field are numerous.
“It’s not demanding like hospital care where you have to be on your feet all the time and deal with all the doctors,” Boone said. “So, it’s really good for a nurse who’s burnt out and still wants to stay in the mix.”
Boone says the payoff for this kind of work comes in connecting with her individuals.
“These people energize me. They fill my bucket,” Boone said. “They become like family.”
Stabilization and Crisis Unit
Linda Martinez
Linda Martinez, an outreach nurse at SACU, had never stopped to consider the elongated lineage of caretaking in her family; there are five generations of nurses and/or nurses’ aides, starting with her grandmother, then her mother, then herself, and her daughter, and most recently, her 19-year-old granddaughter. And that’s not counting her sister and one of her aunts.

“As my mother put it, ‘We’re nurturers,’” Martinez said. “Caretaking is in our blood.”
Although Martinez seemed destined to become a nurse based on family pattern, she wasn’t sure exactly what kind of nurse she would become. She only remembers wanting to pursue this professional path when she was in the 6th grade, after spending countless evenings of her youth listening to her mother come home and recount stories about the patients in her care and the colleagues she worked with, “the funny and the sad,” Martinez said.
“I told my mom I wanted to be a nurse, and she didn’t try to talk me out of it,” Martinez said. “She just said it’s hard work. You have to work long hours. You have to work weekends and nights.”
These warnings failed to deter Martinez.
“I’ve always wanted to work in the medical field somehow,” she said.
It was a line of work that would ultimately slingshot her between both outer edges of the state—eastern and western Oregon.
Martinez, who was born in Pendleton, got her first job after graduating from high school working in a nursing home in Walla Walla, Wash. It was the late 1970s, and though she had made an initial attempt at nursing school after leaving high school, she didn’t finish. Instead, she got pulled further into various opportunities to continue working in the medical field without a degree.
She eventually landed a job working with individuals with I/DD at Eastern Oregon Training Center in Pendleton in 1982, which returned her to her roots. But that year, as Eastern Oregon Training Center was set to close, Martinez was transferred 255 miles away to Fairview Hospital in Salem in 1984, where she worked with individuals with I/DD for the next eight years.
It was around this time that Martinez began to see a clear path to a nursing career and she decided to enroll at Blue Mountain College in Pendleton, her life once again arcing back to her hometown, where she earned an LPN degree in 1999 and her RN degree in 2000. The very next year, she landed a job at Salem’s SACU, crossing the Cascade Mountain range one final time. She has worked at SACU ever since.
After 20 years at SACU, Martinez retired in May 2023, but due to staffing shortages, she was persuaded to return and help fill in for a SACU nurse who had left the agency.
Two of the residential homes where she works have residents under the age of 18.
“When you joke with them or play catch with them, or just say, ‘Hi,’ and spend five minutes with them, it makes their day,” Martinez said.
In her time working with the I/DD population, Martinez said she has been impacted in positive ways; this field has helped her see the humanity in everyone, especially those with disabilities and mental illnesses.
“You have to think of the individual as a person, not their diagnosis,” Martinez said. “Yes, that’s why they’re here, but when you build rapport with individuals and you see them as a person, you can have a great interaction with them.”
In December 2023, she plans to retire for good, leaving yet another nursing vacancy.
“It’s hard to think about leaving,” Martinez said, adding that though her work was sometimes stressful, it was also deeply meaningful.
Challenges of This Kind of Work.
Despite the many rewards that come with working in the I/DD field, nurses say the challenges are real and at times, can be intense. Martinez said more awareness is needed around individuals with I/DD. She hopes people in general and those in the medical field specifically have more empathy with regards to the I/DD population.
Meanwhile, nurses are taking the initiative to help fill their own ranks by targeting the knowledge gap early in the nursing school-to-placement pipeline. Pierce-Green says the wholesale absence of education about the I/DD population for nursing students is a major missed opportunity.
“In nursing school, we did not learn anything about developmental and intellectual disabilities, so that was not on my radar,” Pierce-Green said. “All of your clinical rotations were in ER.”
This knowledge gap has created strain for managers like Duran who are struggling to keep staff positions filled.

“I’m competing against fields people already know about when I’m hiring,” Duran said. “It’s difficult for people to apply to something they don’t know about. We’re trying to plug holes so people don’t end up on the streets because nurses you have in this field are so few.”
Nurses like Duran, Pierce-Green and Boone are currently finding ways to educate nursing students about I/DD as a potential career by working with local nursing schools to include I/DD homes as part of a student’s required rotation before they graduate.
Specifically, Duran and Pierce-Green are working with Chemeketa College in Salem and Boone and her colleagues at Umpqua Homes are coordinating with Umpqua Community College. Boone is also hoping to get Lane Community College to bring back its licensed practical nurse program as part of the range of academic offerings to broaden the base of nurses who would be eligible for jobs in the I/DD field.
Ultimately, nurses who work with individuals who have intellectual and developmental disabilities say it’s not a job for everyone, but it can be a career pinnacle for the right person.
“You have to be self-motivated. You have to be organized. You have to have patience. You need to be able to see the small things and recognize the little joyful moments,” Pierce-Green said. “If you are the kind of nurse who enjoys building relationships and mentoring and have intrinsic environmental awareness and awareness of self, this may be a great opportunity for you.”